08
Jul
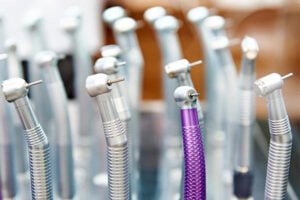
Water Quality and Dental Handpiece Longevity
Dental unit water lines (DUWLs) play an important role in dental practices, as they facilitate the delivery of water to essential tools...
30
May
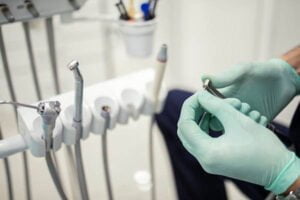
Dental Market Trends: What Dentists Are Looking for in Handpieces
According to Allied Market Research, the projected value of the dental handpiece market in 2031 is an impressive $2.7 billion...
17
Oct
Ceramic vs. Steel Dental Handpiece Bearings: Should You Make the Switch?
Have you considered the role dental handpiece bearings play in your practice’s efficiency and patient satisfaction?
In the world of ...
13
Sep
The Power Play of Speed and Torque In Dental Handpiece Performance
What do dental handpieces, race cars, track athletes, and major league baseball pitchers have in common?
A need ...
01
Aug
How To Properly Store Your Dental Handpieces To Prolong Their Lifespan
Dental handpieces play a pivotal role in the success of your practice, enabling you to deliver exceptional care that your patients rely...
05
Jul
Stay Ahead in Dentistry with 5 Dental Handpiece Trends and Innovations
Whether you’re a newcomer to the dental profession or a seasoned industry veteran, staying informed and current on the latest...
31
May
Exploring the Differences Between Electric and Air-Driven Handpieces
Dentistry is a craft as much as it is a science. While the theoretical knowledge you gained in school and on the job is crucial, the qu...
09
May
Power Up Your Dental Practice: How Proper Suction Line Maintenance Can Improve Efficiency and Safety
In a dental practice, every detail counts.
Customer service is key. Technical skills are paramount. Administrative profici...