As your dental practice begins to welcome patients again, their safety and that of your dentists, hygienists, and the rest of your staff is paramount.
With a heightened public awareness of cleanliness, sanitation, and safety, any hint of poor practices can damage your reputation. Furthermore, you can’t afford to put yourself, your team, and your community in harm’s way.
Since the human mouth is home to 700-plus species of bacteria, and dental practices warrant specific infection control considerations, we all must be vigilant.
Unfortunately, many dentists aren’t protecting themselves or their patients from the potential infections that come with being exposed to those germs, particularly in the form of dental aerosols.
What Are Dental Aerosols? Are They Related to COVID-19?
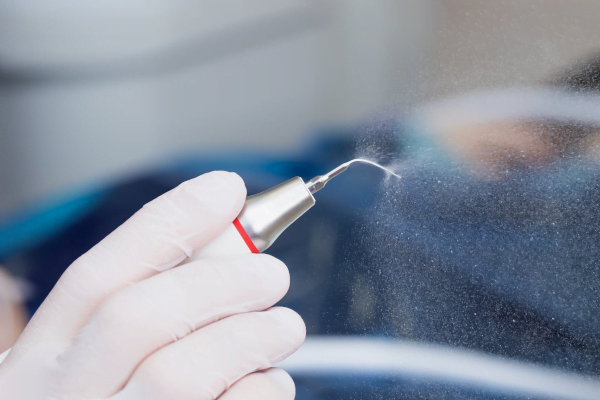
The working definition of a dental aerosol is a solid or liquid particle in a gas, produced during many dental procedures, under 50μm in diameter (anything bigger is classified as splatter.) Dental aerosols are created when scalers, drills, and other high-speed equipment interact with saliva, blood, or plaque.
Although not all dental aerosols are harmful, these airborne materials can contain harmful bacteria and viruses, including COVID-19. Dentists who treat patients using aerosolization are at high risk of infecting themselves, their dental assistants, and others working at their practice.
It should then come as no surprise that dentists find themselves afflicted with respiratory infections more frequently than most, due to the perils of their environment. In addition to concerns regarding COVID-19, there is also proof of aerosols harbouring other cross-infection risks, including the common cold, sinusitis, pharyngitis, pneumonia, tuberculosis, SARS, influenza, and swine flu.
Moreover, harmful pathogens caused by aerosols linger in the atmosphere long after you’ve finished with your patients. In fact, contamination occurs most frequently due to the inhalation of infectious particles after they have settled on surfaces.
Another way aerosol contamination often occurs is when the evacuation system or dental unit waterlines are of poor quality or have been compromised in some way. This can result from water stagnation, inadequate cleaning, heating of your chair unit, and reservoir bottle contamination.
The health risks of aerosols vary between patients, depending on their saliva, blood, plaque, and mucus, and if there’s any infection present.
Managing Aerosols at Your Practice
The perils of aerosols can be mitigated through proactive aerosol management measures, such correct fittings, appropriate level masks, high volume suction, and the use of products that protect the patient’s nasal passages. You and your team should adhere to a comprehensive infection-prevention plan the moment patients enter the practice.
Given that the risk level of a dental aerosol depends on a patient’s health, you should gain a full medical history of your clients. This means completing a thorough examination and making your patient rinse their mouth with a microbial mouth rinse before treatments.
Face masks, of at least ASTM Level 3, should be snugly covering your mouth and nose. Only use a mask for one appointment, switching to a new one for each patient.
Regarding treatment-based equipment, flush lines and reservoirs with a microbial evacuation system cleaner like Bio-Pure. Bio-Pure is a non-foaming, 100% natural cleaner that can be used anywhere there is organic waste and water, including plaster traps, cuspidors, and drains.
Dental aerosols are a major concern for infection control within dental care, especially in light of COVID-19. We hope that this advice will help you and your team feel safer and better prepared to face this post-pandemic world with confidence. Reach out to us to learn more about any of our EPA-compliant cleaning products.